The medical supply chain is the latest fiasco.
As of March 19, the Centers for Disease Control and Prevention (CDC) has reported 10,442 confirmed cases of coronavirus Covid-19 in all 50 states, Puerto Rico, Guam, and the US Virgin Islands.
But the actual number of cases is much higher, experts say — and the main reason we don’t know how big it is is that the government is still way behind in distributing tests to the health providers who need them.
The Covid Tracking Project — where journalists at the Atlantic and scientists are tallying numbers from state public health authorities — says that as of March 20, the US has tested 111,638 people. That’s still far, far short of the million tests promised by the Food and Drug Administration (FDA) in early March.
In most areas of the US, tests are still mainly reserved for hospitalized patients with severe illness, health care workers, or patients involved in a known illness cluster. Some doctors say the ability to expand testing to others is desperately needed.
“As an ER doctor trying to treat patients who may have Covid-19, I can’t underscore enough how much harder the lack of testing is making our job,” Rob Davidson, an emergency physician in western Michigan, told Vox. Since hospital staff have to wear protective gear — which is difficult to work in and, increasingly, in limited supply — for every suspected case, they may be wasting some of it on patients who are negative. Davidson also fears what’s coming next: “With only seven ventilators in my hospital, an overwhelming surge of Covid-19 patients may force me to choose one life over another based strictly on resources.”
/cdn.vox-cdn.com/uploads/chorus_asset/file/19821146/GettyImages_1207811220.jpg) Andrew Caballero-Reynolds/AFP via Getty Images
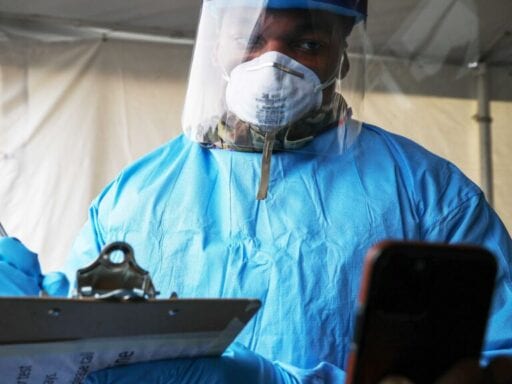
Andrew Caballero-Reynolds/AFP via Getty ImagesAn emergency room nurse in the Seattle area, one of the country’s largest Covid-19 hotspots, who asked not to be identified as she hadn’t been authorized to speak publicly, described the scramble to treat patients who haven’t been tested as “running blind in the ER.” Her emergency department no longer has any masks with face shields, and N95s are in such short supply that they are locked up.
Even some health care workers are struggling to get tested, including one nurse in New York, who also wished to remain anonymous. She told Vox she knows she was exposed while caring for a patient, but was told that she should simply continue working until she showed symptoms. New estimates suggest 20 percent to 30 percent of medical staff in Italy, which has been hard hit by the virus, have been infected, which underscores why testing at scale is incredibly important for the US response.
There’s been a lot of excellent reporting about why the US testing capacity has lagged so far behind: Major hurdles have included bureaucratic challenges and poor communication between laboratories and central agencies
But now that many more labs are able to run tests, the next big problem is the medical supply chain. Here’s what you need to know about the state of testing today.
1) How does a Covid-19 test work?
The most commonly used test is a nasopharyngeal swab, where a special Q-tip is put up your nose to take a sample. This swab is then sent out to a laboratory that can extract the virus’s RNA. The virus that causes Covid-19, SARS-CoV-2, is an RNA virus, which means it uses ribonucleic acid as its genetic material. It requires a process called reverse transcription, or RT, to transcribe its RNA into DNA.
Because there’s not very much material in one sample, a polymerase chain reaction (PCR) is used to rapidly make billions of copies so it can be analyzed. The DNA is dyed a fluorescent color, which glows if SARS-CoV-2 is present. Most of the available Covid-19 tests use this process. The virus has about 32,000 nucleotides, so there’s a variety of tests, each looking for different parts of the virus’s genome, and they use different chemicals — there’s not one test every country is using.
/cdn.vox-cdn.com/uploads/chorus_asset/file/19821177/GettyImages_1212276751.jpg) John Moore/Getty Images
John Moore/Getty ImagesIn the US, the CDC chose not to follow WHO protocol and made its own test, shipping it to states in early February. (The CDC has not made a public statement on why it didn’t follow WHO protocol.) The kit was actually designed to run three tests: two for SARS-CoV-2 and one for other known coronaviruses, which cause many common colds. But laboratories around the country soon reported that the tests didn’t work.
By comparison, German scientists developed the first test for Covid-19 in January in line with WHO protocol, and the WHO shipped 250,000 of these tests to the 60 countries who’d accepted them by early February — saving valuable weeks of being able to identify people who’d been infected.
Despite a nationwide shortage, the need for FDA approval kept local, state, private, or academic institutions from developing or producing their own tests. Although in a crisis the FDA can use something called emergency use authorization to allow unapproved medical tests, they waited until February 29 before actually doing so.
Laboratories in the US all have different equipment from academic research institutions, which are different from those used in hospitals, so Covid-19 tests have to be independently verified in each lab to make sure they’re working right.
Finally, PCR technology has been around for a long time, but it’s time-consuming and complicated to perform, and it’s very easy to contaminate samples. The RT-PCR test itself only takes about a day, but with shortages and the need to ship samples to labs, it’s currently taking most patients days, or even weeks, to get their results back.
2) Are there enough Covid-19 tests in the US now?
The short answer is no. Eight weeks after the US had its first confirmed Covid-19 case, we still don’t have enough tests, both because we are still gaining the ability to process results, and now because the test materials themselves are in short supply.
Until March 9, the CDC required laboratories to test two specimens from each patient, so the number of tests some state health departments said were available didn’t represent the number of patients who could be tested. Patients also often need to be tested multiple times, both to confirm their infection and to be released from isolation.
/cdn.vox-cdn.com/uploads/chorus_asset/file/19821201/GettyImages_1207811150.jpg) Angela Weiss/AFP via Getty Images
Angela Weiss/AFP via Getty ImagesThe good news is that the FDA is now allowing private companies and academic institutions to make their own tests. The pharmaceutical company Roche got approval to develop an automated test on March 13; prior to that, all of the tests had been hand-done. And as of March 19, 89 public health laboratories and even more private ones are finally able to run tests for SARS-CoV-2.
The CDC told Rep. Mark Pocan (D-WI) on March 13 that, nationwide, the US had the capacity to run around 7,000 tests per day; a tracking project run by Scott Gottlieb, a former FDA commissioner, suggests that as of March 18, more than 36,000 Americans can now be tested in a day.
Surprisingly, the CDC is not publicly reporting state-by-state testing capacity — a critical number to understand public health — so it’s difficult to quantify just how much the demand for tests is still outrunning supply, or even to confirm total capacity.
Of the five medical professionals from five different states Vox spoke to, each said that limited supplies were preventing adequate testing in their institutions. For example, the Oregon State Public Health Lab says that they are still limited to 80 tests a day; Oregon Public Broadcasting reports that’s only one out of every 4,555 people.
Some states appear to be rolling out drive-through clinics and other support faster than others. As of March 17, New York had opened at least one such testing facility and has plans for others in at least four counties; Mayor De Blasio announced on the 17th that New York City now had the capacity for 5,000 tests a day. Last Friday, a website intended to help people find testing locations was promoted by President Trump, but it wasn’t actually ready for rollout. In its California debut over the weekend, users found a few bugs: It told patients with symptoms matching Covid-19 they weren’t eligible for screening, it required a Google account, and within hours of launching, its available appointments were full. (Twenty people were tested on the 17th through the program before it too ran out of tests.)
But Scott Gottlieb is optimistic about the upward testing trend, tweeting that this week, “testing capacity will substantially increase nationwide.”
3) What is the primary problem in getting more tests out now?
There have been many missteps in the quest to get an adequate number of tests for Covid-19 patients, including bureaucracy and leadership problems. But now that many labs are able to run tests, says Gottlieb, the problem is the supply chain for the materials.
“We’re going to see a surge in testing over the next few weeks,” says Andy Slavitt, a former Acting Administrator of the Centers for Medicare and Medicaid Services, and a leader of the team which repaired Healthcare.gov after its problematic rollout. “That’s all good, but at some point I expect we will see testing growth slow down again as we run out of supplies.”
It turns out the chemical reagents these tests depend on are in short supply, as well as the plastic vials patients’ samples are transported in, and the swabs used during the testing process. (One of the primary manufacturers of these swabs is in Italy’s hot zone.)
Many suppliers had even less of this critical equipment when the pandemic broke than they normally do because of Trump’s trade war with China. Politico reports that CDC director Robert Redfield says he doesn’t know what the agency would do if RNA extraction kits and reagents become unavailable.
4) Isn’t there a better way to do it?
Probably. PCR is generally considered to be very accurate, but one study suggests that RT-PCR accuracy varies depending on how samples from your nose, throat, or lungs are collected and when you are tested. Only 3 percent of the patients in this study ended up with false negatives — meaning they had Covid-19 but were told they didn’t — but even missing a small number of cases could have deadly consequences.
PCR testing is also slow; under the best of circumstances, it can take a day to get results. Dozens of companies have announced plans to develop a “point of care” test, which a nurse or doctor can use right in their office and get results back in as little as 15 minutes. Some of these tests will also rely on nose and throat swabs and PCR, while others will look for antibodies to the virus in patients’ blood, known as a serological test. This approach could also tell if someone had been previously infected, even if they’re not currently sick. Serological tests are thought to perhaps be less accurate than PCR but are less complicated to perform and easier to automate.
There were no serological tests for Covid-19 until this week when BioAmerica started shipping a new, $10 test to government agencies. Others, like Mammoth Biosciences, plan to use CRISPR to develop a test that works with paper test strips. Still others plan to roll out a $135 at-home PCR test by March 23, with results back in 72 hours.
The primary reason we don’t already have these new testing strategies up and running yet is there hasn’t been a large-scale investment made by companies to commercialize them; until recently, getting FDA approval for new tests was a long process. Now, the FDA is allowing companies to proceed with their diagnostic tests without getting an official clearance — which may bring its own problems. Roche’s test, for example, was approved in less than 24 hours.
5) What problems will testing more people solve?
A March 18 CDC investigation into the Life Care Center, the nursing home at the center of the Kirkland, Washington, outbreak, found that one of the primary problems is that staff weren’t promptly tested, so they continued working after being infected, getting more people in the nursing home sick.
In contrast, the small town of Vo, Italy recently decided to test all 3,300 people, including those who didn’t have symptoms — twice. When the study began on March 6, there were at least 90 people with Covid-19. The comprehensive testing allowed those with the disease to be isolated and those who’d been exposed to be quarantined. As of March 18, there had been no new cases in Vo for days.
/cdn.vox-cdn.com/uploads/chorus_asset/file/19821216/GettyImages_1205351647.jpg) Jason Redmond/AFP via Getty Images
Jason Redmond/AFP via Getty ImagesTom Friedman, a former director of the CDC, says that in areas with few cases, testing helps facilitate contact tracing and inform isolation strategies. Where there is already community transmission, it can help protect vulnerable groups like those in nursing homes, shelters, or prisons. Testing also helps doctors know when it’s safe to discharge patients, and to understand what role people who might be infected but don’t have symptoms are playing in the disease’s spread. Widespread testing may also help keep the economy running, as lockdowns can be targeted rather than sweeping, allowing uninfected people to keep working.
6) What are the limits of testing?
To be effective, testing needs to be paired with actions to slow the spread of the virus. “We have to give the supply chain time to catch up,” says Slavitt. “This is where social distancing is so important.” Many states are now warning that personal protective equipment is in danger of running out, which may reduce the number of health care workers healthy enough to provide care for others. There’s also the concern that widespread testing will expose many health care workers to the virus: When someone sticks a swab up your nose, the natural reaction is to sneeze or cough in their face.
“Testing isn’t a panacea,” Davidson says. “The test isn’t a be-all and end-all. Public behavior is the far more important piece of all of this.” He works nights and is generally the only doctor in the hospital during his shifts. “We’ve all heard the horror stories out of Italy,” he says of his colleagues — of doctors being forced to choose between patients because they don’t have supplies to care for everyone — and they’re concerned the public still isn’t taking the situation seriously enough.
They recommend staying home and away from other people before you get sick, quarantining if you think you’ve been exposed or are asked by a doctor to so, and isolating if you get sick. At this point, some models predict Washington will exceed hospital capacity within the next two days. “For any one doctor or nurse or hospital’s reaction, what people do on their own is much more important.”
Davidson adds, “We’re depending on them to do the right thing.”
Lois Parshley is a freelance investigative journalist and the 2019-2020 Snedden Chair of Journalism at the University of Alaska Fairbanks. Find her on Twitter @loisparshley.
Author: Lois Parshley
Read More