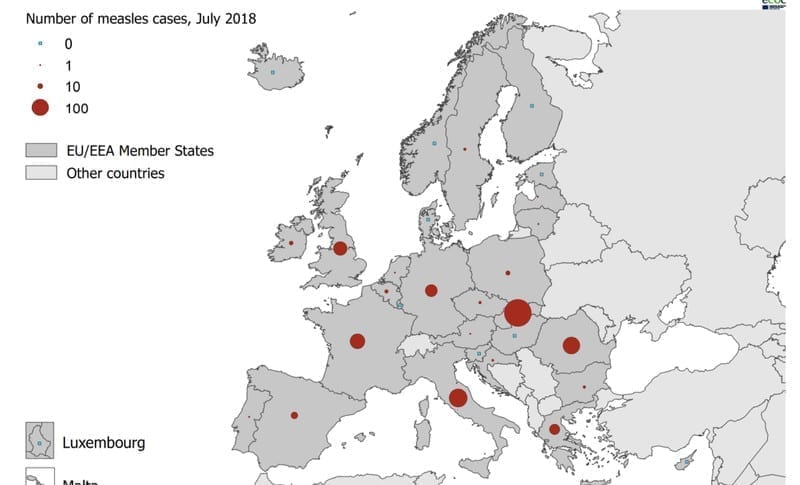
And many countries in Europe are under-vaccinated. “Italy, France and Serbia, for example, have lower child-vaccinations rates than Burundi, Rwanda and Senegal,” the Economist recently reported.
To boost vaccination rates, many countries in Europe have been cracking down on vaccine-refusing parents, experimenting with fines and sanctions. And, to be clear, vaccine refusal is a problem. France, for example, has one of the highest rates of vaccine skepticism in the world: According to one study, 41 percent of people there disagreed that vaccines are safe. In Germany, it’s not unusual to go into pharmacies and find homeopathic “cures” for many ailments, or even homeopathic hospitals.
“The vaccine acceptance issues are a bigger piece of the pie than they were historically,” Larson said.
But Europe’s vaccine problems are much larger than anti-vaxxers. And the story of measles may be the canary in the coal mine for an infectious diseases problem that’s even more dire than it appears right now.
Author: Julia Belluz