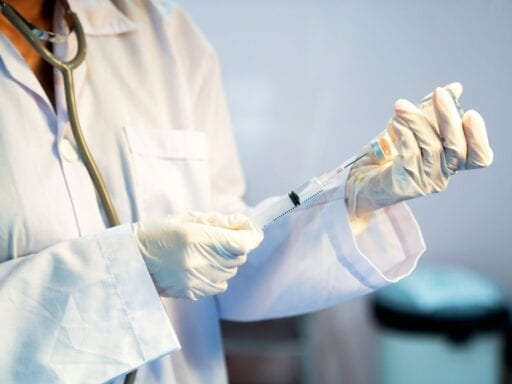
Even my teenage brother and 80-year-old grandma have signed up to help with one of the most consequential medical developments in the world.
Clinical trials for the Covid-19 vaccine began in the United States on March 20. Two days prior, I texted my friends that I wanted to sign up as soon as they began enrollment.
“You know how dangerous that is? That’s why they’re trials!” my friend responded, with genuine concern.
But I wasn’t worried. My father is an oncologist, my mother a clinical-trial researcher. In fact, my entire family — my parents, brother, sister, grandmother, and I — signed up for the Pfizer BioNTech vaccine trial. I feel safe because I am informed about the risks, because I know ethical considerations have been made, and because I trust my mom and dad’s recommendations as medical professionals — and as my parents.
I get why there’s a perception that human clinical trials are unsafe, or that enrolling in a trial is like consenting to be a lab rat. Medications and vaccines in trials have not yet been FDA-approved, and that idea alone is scary. How good can a new medicine be if we’re still trying to prove that it’s safe and it works? Plus, if we don’t even know all the possible side effects yet, how do we know what to expect?
It doesn’t help that in the United States, there is already unwarranted skepticism and fear around vaccines. President Donald Trump’s declaration that he would get a vaccine approved before Election Day has raised fears about whether he can actually bypass standard medical and clinical regulations and distribute a vaccine before it’s ready. (Fact-check: He can’t.) The politicization of brand new vaccines has resulted in a lot of confusion and doubt: Less than 50 percent of Americans say they are committed to getting a Covid-19 vaccine when it becomes available.
There’s a lot of misinformation and disinformation in 2020, and the Trump administration has interfered in the decision-making of public health institutions like the Centers for Disease Control and Prevention and the Food and Drug Administration (FDA). For many Americans, it’s gotten more difficult to know who to trust and what to believe about a contagious virus we still have so much to learn about.
But the process of developing a vaccine at unprecedented speed has actually been a rare success story in the US pandemic response, and trials like what I’m participating in are an important way to make sure vaccines are safe. When I asked my mother, Vicky, a clinical-trial researcher, to explain to me how this would work, she stressed that the most essential element of a vaccine trial is “preserving the safety of the individual, first and foremost.” Knowing this, I decided to sign up to test out one of the most consequential medical developments in the world right now.
What happens during the Covid-19 vaccine trial?
As the coronavirus spread throughout Florida, where we live, my family spent less and less time leaving the house. Like many families, we were getting groceries delivered and limiting our contact with people. My mom, sister, grandmother and I were all working from home. We were being as safe as we could, but there were still some concerns. My brother was about to start in-person school. My dad works in a hospital and treats immunocompromised patients, which puts him at risk for Covid-19.
However, his being a doctor also means he is considered a priority for the vaccine trial. My grandmother, because of her age group, was also considered a priority. And because we all lived together for the summer, it made sense for all of us to enroll, to protect each other.
/cdn.vox-cdn.com/uploads/chorus_asset/file/21985273/Family.jpeg) Courtesy of Vicky Hajdenberg
Courtesy of Vicky HajdenbergNearly 30,000 people nationwide are expected to participate in the study. But trials are only conducted in cities where the virus is spreading. In Orlando, Florida, where we enrolled, daily new cases of Covid-19 reached a peak of more than 15,000 by mid-July. Statewide, the virus was on the rise as well.
Over a period of about three months, the six of us received two injections spaced three weeks apart. Four weeks after the second injection, we went back for another blood draw, which the investigators will use to check how many antibodies we produced. Because the study is randomized and observer-blind, the researchers, doctors, and participants do not know who received the vaccine and who received the placebo. According to the consent form, we could be in this study for up to 26 months and will need to visit the site another three or four times. Over the course of the study, we will have had our blood drawn five times. (On October 16, Pfizer CEO Albert Bourla wrote in an open letter that it is possible we may know whether the vaccine works by the end of October, adding that Pfizer will apply for emergency use authorization by late November, assuming positive safety data.)
In phases 2 and 3 of the Covid-19 trial we enrolled in, the vaccine is given to reasonably healthy individuals. As with other vaccines, it’s meant to be preventive. Plus, this phase of the Pfizer trial merely tests the efficacy of the vaccine against a placebo. Nobody is getting injected with live virus (the stuff that makes you sick); it’s just the mRNA of the protein of the virus.
Throughout the process, there’s careful oversight: An independent committee of experts called a Data Safety Monitoring Board routinely analyzes the safety of a trial. At a minimum, my mother says, these committees are made up of a highly qualified ethicist, physician, and statistician.
In this trial, it appears that no news is good news. There’s not much communication with the clinic unless we need to report symptoms. Follow-up is simple; in fact, we could do almost all of it from our phones. At the end of the first appointment, we were instructed to download a symptom-monitoring app called the Covid-19 Illness Diary, which offers the prompt: “Have you experienced any of the following?” followed by a short list of symptoms. And that’s it. I fill mine out on Mondays.
The appointment for the second injection was nearly identical to the first: I sat in the waiting room, answered questions about my health, took a pregnancy test (required for anyone who can get pregnant), sat in another waiting room, received the injection, and waited for another 30 minutes to monitor symptoms before I was dismissed.
I felt safe the whole time. But I’m also young, and younger people have been shown to be less likely to get seriously ill from Covid-19. And although many older people might be anxious to participate in a trial, my 80-year-old grandmother, Henie, is fairly confident in the process because she is doing it with her family and because she trusts my parents when it comes to science. She also gets to spend some time with my dad when they get their vaccine injections together. Henie said she felt safe at the clinic but also knew the benefits, for her at least, outweighed the risks.
/cdn.vox-cdn.com/uploads/chorus_asset/file/21985280/Henie_and_Dad_and_uncle.jpg) Courtesy of Vicky Alejandro
Courtesy of Vicky AlejandroShe explains that she knew some people who hadn’t left their homes for more than 140 days, and worries that kind of isolation could be more dangerous for someone her age than masking up and participating in the trial in a sterile environment. “And my family participated,” Henie added. “By myself, I don’t think I would have gone.”
Distrust in clinical trials is nothing new
In the US in 2020, there are so many regulations in place that you’d be hard-pressed to find a clinical trial that’s outright dangerous. Events like the International Harmonisation Conference established ethical and safety guidelines, and agencies like the FDA, the US Department of Health and Human Services, ethics committees, and institutional review boards all play a role in creating safeguards for clinical studies. But it’s important to note that before new drugs are ever tested in humans, they are tested in animals first.
There is one caveat, though: In phase 1 trials, a small number of highly at-risk patients, often with terminal illnesses, will enroll in a first-in-humans study to rule out toxicity, or to at least demonstrate the medication is less damaging than the disease itself. But this is not the case with phases 2 and 3 of the Covid-19 vaccine trials, which is what my family and I are participating in.
Understandably, the history of unethical practices, forced and unnecessary procedures, and the absence of consent in medical procedures have left some Black and brown Americans distrustful of such trials — Covid-19 trials in particular do not have enough Black participants because of this legacy, though the Pfizer trial made some headway this summer. (My family members and I in the trial are white and Hispanic.)
My mother is clear to distinguish past abusive experiments from clinical studies today. As she puts it, those experiments “did not intend to protect human subjects.” With the Tuskegee syphilis study, for example, it was already known that there was a cure for syphilis. The study’s organizers were observing the course of a disease as it made its way through an at-risk population, under the guise of providing “free health care” to Black men.
On the other hand, clinical trials have also excluded whole categories of people: minors, pregnant women, and people with disabilities, leaving them at high risk when they take the medicine later. Even my brother, who is 17, was not allowed to participate in the trial until about a month ago. But the moment minors were accepted into the study, my parents signed Jimmy up. “I was like, ‘Okay, cool,’” Jimmy told me.
Informed consent is central to conducting these trials. For our trial, everyone in the room was given an iPad and had to spend about 20 minutes swiping through an informed-consent module explaining how a clinical trial works and the possible risks of the vaccine. I actually developed a very low-grade fever — 99.8 degrees at the highest — after the second shot, though the study directors said it didn’t count because it was below their official threshold for “low-grade fever.” I recovered in less than a day, thankfully. But the decision to participate should be an informed one made by the participant or a legal guardian.
As my mom puts it, “We [had] a sort of a discussion in our family, even before the trial was available, that what we knew of the disease was much more deadly and dangerous than what a vaccine could offer.”
It’s also critical to remember that nobody — including the doctors, who have anonymized all the participants — knows whether they got the vaccine or the placebo. Who got injected with what won’t be revealed until the study is completed. But some of us have our suspicions.
My grandmother is convinced she got a placebo. She says she had no side effects whatsoever: “It was like drinking a glass of water.”
Jackie Hajdenberg is an investigative reporter with Columbia Journalism Investigations and USA Today, focusing on voter access. She is based in New York City and Central Florida.
Millions turn to Vox each month to understand what’s happening in the news, from the coronavirus crisis to a racial reckoning to what is, quite possibly, the most consequential presidential election of our lifetimes. Our mission has never been more vital than it is in this moment: to empower you through understanding. But our distinctive brand of explanatory journalism takes resources. Even when the economy and the news advertising market recovers, your support will be a critical part of sustaining our resource-intensive work. If you have already contributed, thank you. If you haven’t, please consider helping everyone make sense of an increasingly chaotic world: Contribute today from as little as $3.
Author: Jackie Hajdenberg
Read More