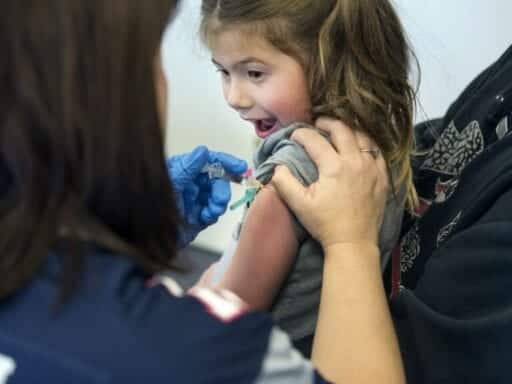
Research is mounting that shows the vaccine’s effectiveness declines over time. Late October may be your best bet.
We’re entering the season of coughing and bodily aches and pains. And if you haven’t been immunized yet, now might be the perfect time to get a flu shot.
Though flu vaccine campaigns begin as early as August, several studies published in recent years show the flu vaccine’s effectiveness actually declines over time in the months after the shot is given. So if you immunize too early, you might lose some — or all — immunity by the time flu season is peaking in January and February. (If you already got your flu shot, there’s not much you can do this season, but remember this advice next time flu rolls around.)
Getting vaccinated a little later — around the end of October — can protect you through the height of flu activity. To understand why, let’s take a look at recent studies of how vaccine protection changes during a flu season.
Why people who vaccinate too early may be more likely to get the flu
In one 2017 study, researchers from the Centers for Disease Control and Prevention looked at data from four recent US flu seasons to track whether and when the vaccine’s effectiveness starts to wane.
They found the shot was most effective just after vaccination, followed by a drop off that varied slightly by the type of flu virus. (There are four kinds of influenza viruses — A, B, C, and D — and seasonal flu is caused by influenza A and B. Every year, different strains of these pathogens circulate.) So for influenza A(H3N2) and influenza B, the vaccine’s effectiveness dropped 7 percent per month after vaccination. For influenza A(H1N1), it dropped 6 to 11 percent per month.
Overall, the researchers said, “We observed decreasing influenza vaccine protection with increasing time since vaccination across influenza types/subtypes.”
Another 2018 paper looked at even more flu seasons — seven — and found a similar pattern: “Across all seasons, every additional 28 days between vaccination and influenza testing was associated with, approximately, a 16 percent increase in the odds of testing positive for any influenza.” This finding was driven mostly by the waning of influenza A immunity, the authors — most of whom are at Kaiser Permanente — wrote.
Other recent papers have come to similar conclusions — such as a UK study of the 2011–2012 flu season, and a study from Spain that found a drop off in vaccine effectiveness to zero 119 days after vaccination.
“Though the root causes of intraseasonal waning immunity are up for debate … the evidence towards its existence is becoming increasingly difficult to ignore,” wrote a pair of researchers in a 2018 journal Clinical Infectious Diseases editorial, cheekily titled “Early bird gets the flu.” They note that there’s a lot we still have to understand about this phenomenon — how it differs among age groups, or people with certain underlying diseases that affect the immune system, such as HIV.
But for now, the editorial authors wrote, “The prospect that a vaccine administered in August loses effectiveness in as little as 3 or 4 months is troubling.” That’s because “the millions of people who are vaccinated in August and September may be at risk by January or February, historically when influenza season peaks.”
So what does this mean for people who already got vaccinated? There’s not much you can do this year. CDC says there’s no benefit to vaccinating twice in a season, and the Advisory Committee on Immunization Practices, which sets vaccine policy in the US, hasn’t changed its guidance yet to reflect the new research. They currently recommend getting vaccinated by the end of October, and this year warned, “Vaccinating early — for example, in July or August — may lead to reduced protection against influenza later in the season, particularly among older adults.”
There are many good public health reasons to get vaccinated against flu
As we’ve reported before, flu vaccines carry very little risk — and the big potential benefit of avoiding serious illness for you and those around you. That’s because getting the vaccine isn’t only about protecting yourself; it’s about protecting others through herd immunity. When enough people are immunized, the virus is less likely to spread. So even if you think you can shrug off a bout of influenza, you could spread it to more vulnerable people who can’t.
Older people, young children, pregnant women, and people with compromised immune systems are particularly vulnerable to influenza. So herd immunity and the vaccine is especially important for these groups. During the 2017-2018 flu season, 80 percent of pediatric deaths occurred in unvaccinated children, according to the CDC.
As for treating flu, most people can just wait out their sickness at home, getting lots of rest and taking care not to infect others. But people in those high-risk groups — young children, pregnant women, people over age 65, those with other chronic diseases — may want to seek immediate medical attention and antivirals like Tamiflu.
In the meantime, there are other, even simpler things you can do to mitigate your risk of getting the flu or spreading the virus to others. They include good old-fashioned hand-washing, covering your mouth when you cough, and, again, staying home if you’re sick.
Further reading
- Flu season 2018: why it got so bad
- How Linus Pauling duped America into believing vitamin C cures colds
- The flu vaccine isn’t perfect — but that doesn’t mean you should skip it
- Cold versus flu, explained
Author: Julia Belluz
Read More